
Dear World,
We all crowded around, and I remember telling them as I watched the heart rate on the monitor, “this is it.”
︎
If you’ve been reading about what it’s like in ICU treating COVID patients, you know that families can’t come to say goodbye to their loved ones.
This, as you might imagine, is devastating for the families who can’t come, but also strikes a sadness within us as nurses.
For me, it’s also given me a gift. I know this sounds strange, but let me explain.
My mother died in the same hospital and in the same ICU that I work in. Actually, nurses who work with me cared for my mom and comforted me as a family member. She passed away in September of 2018, and I’ll never forget our last days together.
She loved the beach. As she progressed in her battle with lymphoma, my family and I thought it would be nice to take her to the beach. The lymphoma had moved to her brain. She said, “I want to fight,” so we let her continue treatment options to let her fight, but they weren’t working.
She hadn’t spoken in days. While at the beach, she took a turn for the worst, and we needed to get her back to Louisiana to my hospital where her doctors were. I remember her head laying in my lap in the back of the car on the way home. I remember thinking: Mom, please don’t die on an interstate in Alabama. Please don’t die in my car.
We made it to the hospital. My nurses made my family and I feel so comfortable. When we made the decision to switch her care to comfort-focused, we invited the whole family over to the hospital on the day that I knew would be her last.
Picture a hospital room. There’s room for about 15 people in it. A bay window is built into an internal wall so nurses and physicians can look into the room from the hallways. There’s cards, flowers and pictures adorning the tables and nooks of the room.
Next to her bed is a machine that monitors her heart rate.
We’d all been exchanging stories, taking turns talking to her one-on-one. And while my family was watching her--none are medical professionals--I kept watching that monitor. She held steady for that entire day, but as it neared 1:30am the next, a year and one day since her diagnosis, I watched her heart rate…
60 beats per minute went to 40 beats per minute, 40 went to 10.
I asked the family to gather around her bed and to hold her. We all crowded around, and I remember telling them as I watched the heart rate on the monitor, “this is it.”
Asystole--that’s the medical word for flatline.
She left. Back then, I never would have thought that I would be so grateful to have had my family there. It was one of the saddest moments of my life, but I am forever grateful to have been there.
︎︎︎︎
I’m now a charge nurse. Basically, I’m in charge of nurses when I’m on shift. I work one-on-one with the nurses who work with the patients to make sure the ICU unit is running smoothly. In recent weeks, it’s been all hands-on deck. It’s been nice in the sense that I’m remembering why I love nursing.
There was an 81-year-old man in my unit whose kids couldn’t see him. Whose wife was also COVID positive. She refused to see him because she didn’t want to get anyone sick.
He was all alone.
Except for my nurses.
I was in the hallway, looking through one of the internal bay windows.
I watched the monitor: 60..40...10…
My nurses stood on both sides of the bed. Each holding him as he went.
Asystole.
And I cried. There in the window. It sent me back to my mother’s bedside. My mother’s last moments where everyone close to her held whatever piece of her they could as we squeezed together.
In that window at that moment I thought, in what lifetime would family not be able to crowd around their loved one's bed as they died?
This one.
Sincerely,
The Heart Rate Went 60, 40, 10...
Heather Rouyer︎︎︎︎
P.S.



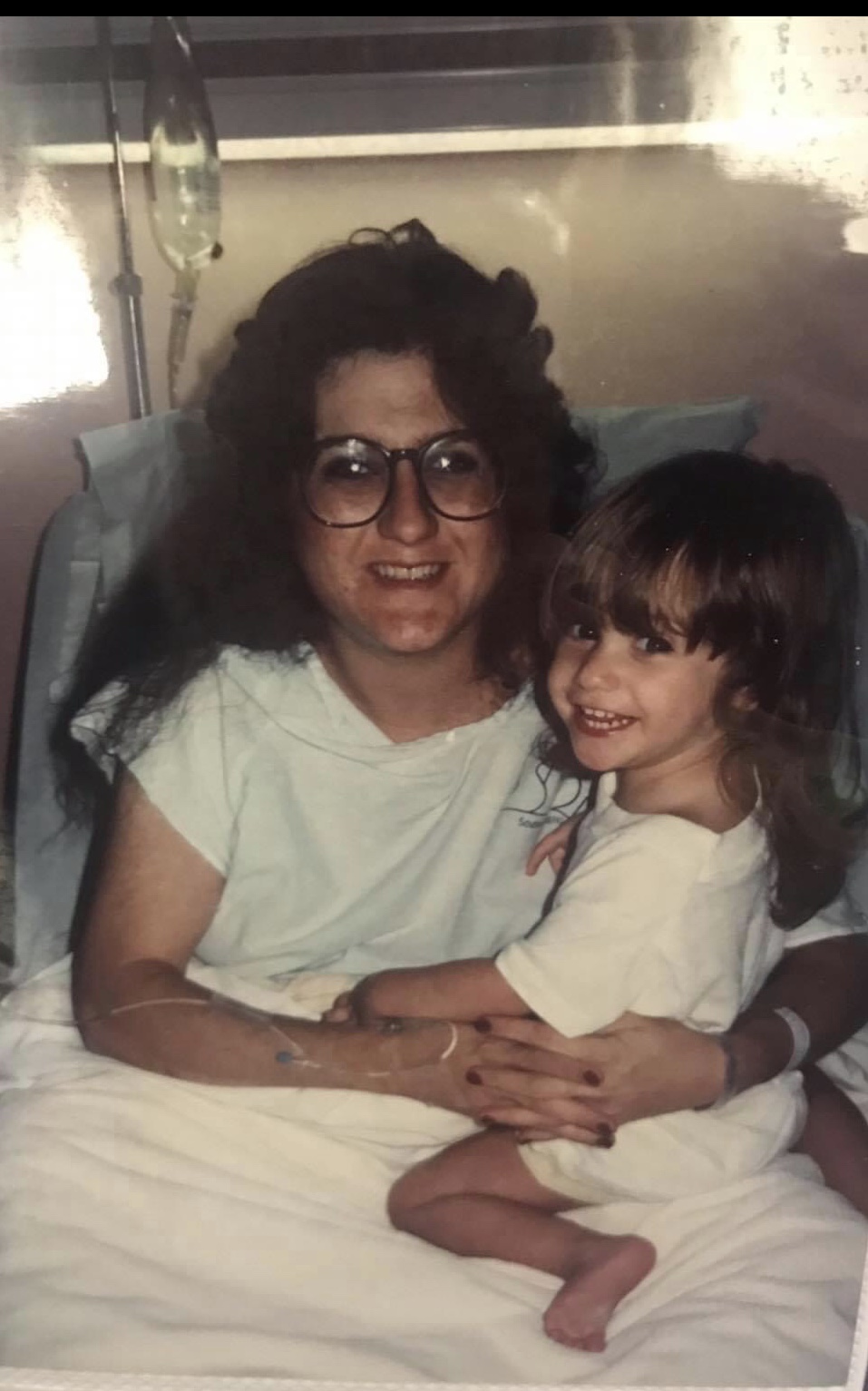


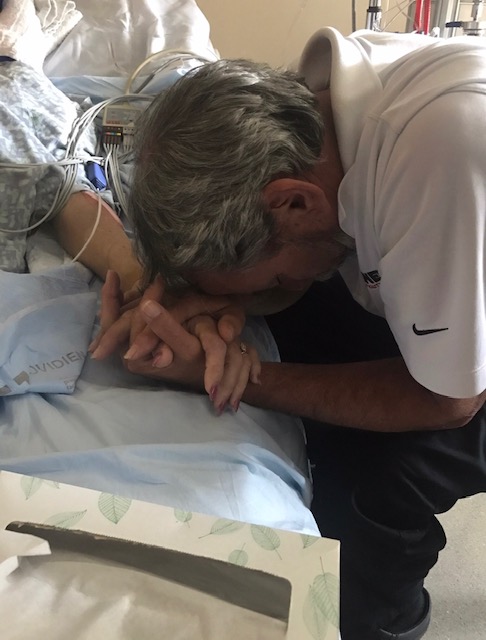
︎︎︎︎
Explore All Stories
︎︎︎︎
contact us
hello@dearworld.org
learn more
dearworld.org
Copyright © 2020 Dear World, Inc.